
In Part I and Part II of this series, I established the following:
(Skip to Part IV.)
- Hunger is not a singular motivation: it is the interaction of several different clinically measurable, provably distinct mental and physical processes.
- In a properly functioning human animal, likes and wants coincide; satiation is an accurate predictor of satiety; and the combination of hunger signals (likes and wants) and satisfaction signals (satiation and satiety) results in energy and nutrient balance at a healthy weight and body composition.
In other words, we shouldn’t have to be hungry all the time in order to stay healthy and fit.
Yet this is clearly not the case. Most diets depend on restraint…and most diets fail.
American Psychologist, Vol 62(3), Apr 2007, 220-233.
Medicare’s search for effective obesity treatments: Diets are not the answer.
Mann, Traci; Tomiyama, A. Janet; Westling, Erika; Lew, Ann-Marie; Samuels, Barbra; Chatman, Jason“The authors review studies of the long-term outcomes of calorie-restricting diets to assess whether dieting is an effective treatment for obesity. These studies show that one third to two thirds of dieters regain more weight than they lost on their diets, and these studies likely underestimate the extent to which dieting is counterproductive because of several methodological problems, all of which bias the studies toward showing successful weight loss maintenance.
In addition, the studies do not provide consistent evidence that dieting results in significant health improvements, regardless of weight change. In sum, there is little support for the notion that diets lead to lasting weight loss or health benefits.”
Am J Clin Nutr. 2009 July; 90(1): 33–40.
Dieting, restraint, and disinhibition predict women’s weight change over 6 y
Jennifer S Savage, Lesa Hoffman, and Leann L Birch“Women who reported dieting at study entry were heavier at study entry and gained more weight over time than did nondieters.”
Appetite. 2006 Jul;47(1):83-90. Epub 2006 May 2.
Multiple types of dieting prospectively predict weight gain during the freshman year of college.
Lowe MR, Annunziato RA, Markowitz JT, Didie E, Bellace DL, Riddell L, Maille C, McKinney S, Stice E.“…Both a history of weight loss dieting and weight suppression (discrepancy between highest weight ever and current weight) predicted greater weight gain, and these effects appeared to be largely independent of one another.”
Why is this?
The flip answer, of course, is “because they’re not eating a paleo diet“. But both the evidence and common sense support a more fundamental conclusion: most diets depend on restraint—known colloquially as “willpower”.
What Is “Willpower”?
Just like the four hunger drives, “willpower” is a provably distinct mental and physical process.
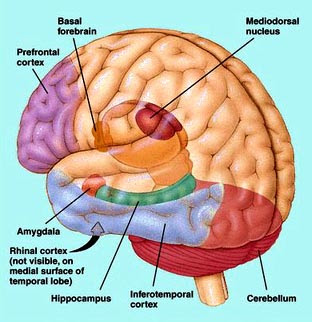
This is your prefrontal cortex.
“…The prefrontal cortex is more developed and extensive in humans than any other primate, and it is responsible for what is called “executive function.” That is, the PFC helps us predict outcomes, prioritize, modulate our emotions to socially acceptable norms, and helps us sort out the best options given conflicting data (reasoning, basically). It is a bit like a policeman for your brain…”
–Dr. Emily Deans
The prefrontal cortex is responsible for what we call “willpower”—our ability to do something we don’t want to do. Willpower is the confounding factor in analyzing hunger motivations, because it can override them…to a degree.
When Willpower Fails (And Diets Fail)
When our wants overcome our will, we call them “needs”.
As anyone who’s tried to learn to play a musical instrument knows, our prefrontal cortex, our “rational mind”, is not fully in charge. All we have to do is put our fingers here, then here, then here…what’s so hard about that? Yet it takes endless hours of practice, because our PFC isn’t even in full control of our fingers—let alone our hunger drives. Similarly, when our wants overcome our will to avoid unhealthy food (or too much food), we will eat regardless.
Unfortunately, most mainstream diets require substantial willpower—huge inputs from the prefrontal cortex—to maintain. This is why the majority of people regain more weight than they lose on a diet: the diet does not bring the four drives of liking, wanting, satiation, and satiety back into balance. It simply depends on an increase in willpower…
…an increase that is, in the long run, not sustainable. The PFC can only influence behavior so much and so often, which is to say that we only have so much willpower.
Stated in plain English:
Most diets fail because they rely on willpower to override our other drives.
Willpower Requires Energy
Skeptical? Here’s the proof: exerting willpower takes a measurable amount of energy!
J Pers Soc Psychol. 2007 Feb;92(2):325-36.
Self-control relies on glucose as a limited energy source: willpower is more than a metaphor.
Gailliot MT, Baumeister RF, DeWall CN, Maner JK, Plant EA, Tice DM, Brewer LE, Schmeichel BJ.Laboratory tests of self-control (i.e., the Stroop task, thought suppression, emotion regulation, attention control) and of social behaviors (i.e., helping behavior, coping with thoughts of death, stifling prejudice during an interracial interaction) showed that (a) acts of self-control reduced blood glucose levels, (b) low levels of blood glucose after an initial self-control task predicted poor performance on a subsequent self-control task, and (c) initial acts of self-control impaired performance on subsequent self-control tasks, but consuming a glucose drink eliminated these impairments. Self-control requires a certain amount of glucose to operate unimpaired. A single act of self-control causes glucose to drop below optimal levels, thereby impairing subsequent attempts at self-control.
And here’s the popular version, from the New York Times.
Right away we can see a problem: impaired blood glucose control, such as we see in diabetes and prediabetes, would exacerbate this effect…so the more we impair our metabolic flexibility by continually stuffing ourselves with carbohydrate, the more trouble we’ll have sticking to our dietary decisions!
Unless (as the study shows) we drink a 120-calorie glass of Kool-Aid, which helps us restrain ourselves from…ingesting sugary junk. Is anyone seeing another problem here?
Why Dieting Makes You Fat: You’re Depending On Willpower
All this seems like an obvious, common-sense result. We know intuitively that willpower is a limited resource: we only have so much tolerance for denying our own wants. Furthermore, life is far more pleasant when we’re not living in a constant state of self-denial (or self-flagellation).
But there are even more reasons to minimize the role of willpower in a diet. These titles say it all, and I don’t even have to quote abstracts:
Am J Clin Nutr. 2001 Jan;73(1):7-12.
Cognitive dietary restraint is associated with higher urinary cortisol excretion in healthy premenopausal women.
McLean JA, Barr SI, Prior JC.J Gerontol A Biol Sci Med Sci. 2006 Jun;61(6):628-33.
High cognitive dietary restraint is associated with increased cortisol excretion in postmenopausal women.
Rideout CA, Linden W, Barr SI.Psychosom Med. 2010 May; 72(4): 357–364.
Low Calorie Dieting Increases Cortisol
A. Janet Tomiyama, Ph.D.,a Traci Mann, Ph.D.,b Danielle Vinas, B.A.,c Jeffrey M. Hunger, B.A.,b Jill DeJager, MPH., RD,d and Shelley E. Taylor, Ph.D.c
In other words, restraint—using our willpower—doesn’t just use energy. It causes stress.
A Brief Note On Cortisol
Cortisol is a glucocorticoid—a class of necessary regulatory hormones whose functions and interactions are far too complicated to discuss here. However, we know that persistently high cortisol levels are strongly associated with increased stress, and that administration of exogenous glucocorticoids (the fancy term for “giving them as drugs”) actually produces increased stress, along with a litany of terrible side effects.
“Side effects of oral corticosteroids that are used on a short-term basis include: an increase in appetite, weight gain, insomnia, fluid retention, and mood changes, such as feeling irritable, or anxious.
Side effects of oral corticosteroids used on a long-term basis (longer than three months) include: osteoporosis (fragile bones), hypertension (high blood pressure), diabetes, weight gain, increased vulnerability to infection, cataracts and glaucoma (eye disorders), thinning of the skin, bruising easily, and muscle weakness.”
–UK National Health Service
Persistently high cortisol not only makes you feel stressed, with all the nervousness, sleep disruption, and ugly side effects that entails…
…it makes you eat!
Psychoneuroendocrinology. 2010 May; 35(4): 607–612.
CRH-stimulated cortisol release and food intake in healthy, non-obese adults
Sophie A. George, Ph.D., Samir Khan, Ph.D., Hedieh Briggs, M.S.W., and James L. Abelson, M.D., Ph.D.“Low dose CRH [corticotropin-releasing hormone] administration significantly increased food intake compared to a placebo injection in healthy, non-obese adults, as measured by both calories and total grams consumed. The magnitude of the peak cortisol response to CRH was a strong predictor of subsequent food intake.
These data extend growing evidence of a link between stress response systems and human eating behavior, by suggesting that activity within the HPA axis – our central, neuroendocrine stress response system – is neurobiologically linked to food consumption.”
Note that George et. al. is an actual controlled study, not an associative population study…so we can conclude that there is a causal relationship, not just an association. Cortisol makes you eat, as do the other corticosteroids…as anyone who has taken prednisone for an extended period of time can tell you.
And since this paper does such a great job of summarizing the literature on glucocorticoids, I’ll simply quote it here:
Glucocorticoids also influence behavior and may further influence energy availability by altering food intake. In humans, chronic GC administration increases ad libitum food intake (Tataranni et al., 1996). In animal models, GCs appear to impact caloric intake through direct neuropharmacological effects (Dallman et al., 2007), and corticosterone has been shown to dose-dependently increase intake of palatable foods such as sucrose, saccharin (Bhatnagar et al., 2000), and lard (la Fleur et al., 2004). These findings may have relevance to the modern obesity epidemic – repeated stress-related GC release could cause excess intake of high calorie foods and contribute to weight gain. Indeed, animals prone to obesity have been shown to need circulating glucocorticoids in order for it to occur (Bray 1985) and GC receptor antagonism prevents or reverses weight gain in these animals (Okada et al., 1992). Interestingly, in humans, there is also a link between heightened HPA axis response to stress and abdominal obesity (Epel et al., 1999; Epel et al., 2000; Pasquali et al., 1993; Pasquali et al., 1999).
–Ibid.
Here’s a tidbit they missed, from a study on cortisol inhibitors in humans that found completely negative results from medicating cortisol levels downward…
…thus proving, once again, that these chemicals are metabolic markers, not control levers we can pull to produce a desired result. Artificially medicating one element of a complex homeostatic system doesn’t always fix a disequilibrium. In other words, you can’t fix your car by removing the “Check Engine” light.
Physiol Behav. 1993 Oct;54(4):717-24.
The effects of the acute administration of RU 486 on dietary fat preference in fasted lean and obese men.
Kramlik SK, Altemus M, Castonguay TW.“…There was a positive correlation between urinary free cortisol and fat intake in obese men during placebo periods when the product chosen was consumed.”
Conclusion: A Successful Diet Must Minimize The Role Of Willpower
The problem here should be obvious:
- Restrained eating causes stress. Continually exercising your willpower in order to eat less food than you want—or different food than you want—is stressful.
- Stress makes you eat more.
Unfortunately, in a world of supernormal stimuli, we can never completely disconnect our prefrontal cortex—because we’ll end up with a long roll of lottery tickets, as well as a shopping cart full of Cheez-Its and Mountain Dew…
…but it’s clear that we need to minimize its role, by bringing our two hunger drives (likes and wants) and our two satisfaction drives (satiation and satiety) as close as we can to their natural evolutionary state of balance and accord.
I’ll continue this series next week with an examination of several different pathological states of hunger, and how they can be explained by the interaction of these four motivations. Click here to continue!
Live in freedom, live in beauty.
JS
Continue to Part IV: When Satiety Fails.
Or, go back to Part I or Part II.
I’m proud of this one. Do you agree? Then share it with the buttons below!


Nice analogy, JS. Wait, I’m not sure it is even an analogy.
Any physical skill has to move from the conscious part of the brain to “muscle memory” to become proficient. I would even extend that to mental skills like solving mathematical problems, the toolbox of things like power series, Euler’s equation, etc, become second nature.
In the same way, a behavior we engage in constantly, such as eating, must include plenty of second nature behavior.
This series is getting more and more interesting. Thanks. Looking forward to the next installment.
As Sean said above, reminds me of strength training and neuro-muscular efficiency:
most people get stronger rapidly and can even improve linearly (normally accompanied by an increase in muscle mass) but later they have to improve neurally to progress.
seems related basically.
interesting write up btw, i have introduced a number of friends to your blog too and they have liked it 🙂
(one has said there was too much science for her. typically this person is moaning about her weight all the time and refuses to learn anything. i give up)
Oh, my – there’s so much to comment on this post, I scarcely know where to begin. Being neither premenopausal nor postmenopausal (yes, I am smack dab in the middle of the peculiar Hell known as perimenopause), I wonder what my cortisol levels look like. They’re far less than they used to be, I can tell you that – removing NADs from my diet has done wonders for the murderous mood swings I used to experience. It’s funny, too, because shortly after I moved to northeast Ohio, which is one of the most overcast areas in the country (I was born and raised in Texas), I was diagnosed with Seasonal Affective Disorder. For the first four winters I was impossible to live with by February. This last winter, though? More or less smooth sailing.
This doesn’t even begin to address the fact I no longer think about food constantly. Well, okay, I think about food all the time, it’s what I do, but I don’t think about eating constantly. So don’t tell me diet isn’t at root of our society’s growing health problems. I’ll laugh in your face.
BTW, JS – just received your book; I’m not far into yet, but I am enjoying it immensely so far.
Wow. I'm blown away.
Great article. This actually explains a lot – especially in the fitness world. It also explains why 'carb refeeds' work. They help to normalize cortisol and every other benefactor by increasing the reward metrics.
Sean:
That's why this issue is so complicated: “force of habit” can convert, partially or in total, a conscious decision originating in the PFC into a habitual behavior driven by other parts of the brain. Which means that, as I pointed out in the previous installment, conscious decisions can not only override the hunger drives, it can modify them to some degree.
But only to some degree. No amount of willpower will make ice cream taste bad, and nothing will make unripe persimmons taste good.
Anand:
Thank you! Now that the groundwork is laid, we can actually start drawing conclusions.
eddie:
My posts vary dramatically in technical content: this latest series is relatively dense. Perhaps I should do a “For Beginners” section in the index that gives new readers a few starting points: do you have any thoughts on that? (Besides “Eat Like A Predator”)
And thanks for spreading the articles! I try to write them so they're understandable to people who aren't already paleo.
Jan:
I'm just getting started here…the next two articles will give you even more to chew on. I'm glad you're enjoying TGC!
Chris:
You're absolutely correct: high cortisol is a major part of overtraining, and it affects a lot more than just hunger. Maybe I'll write about some of those other ramifications someday…but you've already got the drift.
All these issues are connected, and sometimes it's hard to write an article without it spinning out of control into a book!
JS
I'm pretty sure I'd buy that science filled book 🙂
Thanks for the excellent post.
I've also seen something come up a lot more recently, it seems to die down every few years and comes back, about the “Blood Type” Diet. I've never (entirely) bought into it. But it seems to coincide a lot with Paleo Principles.
This has been a fascinating series, but the above is my favorite installment yet. JS, you are doing a great job of keeping these articles succinct and profound.
I didn’t know that acts of self-control actually affect blood glucose levels. This helps explain the late-night binge phenomenon: the mind wills the body to stay awake, lowering blood glucose and driving up cortisol, leading to snowballing hunger and disintegrating self-control. Personally, I have plenty of willpower during the day to make rational food choices, but keep me up past my usual bedtime and I am easily reduced to zombiehood, my hand reaching of its own accord for the salted macadamias…
In her intriguing blog entry from which the quote above, Emily Deans describes a study on pigs. Those pigs that ate junk food to the point of obesity presented decreased PFC activity. So the mental “policeman” atrophies to its weakest when its discipline is needed most. Count that as another strike against willpower as a method of weight loss.
In my own failed diets of the past, relying on willpower was a very ineffective and unpleasant tactic. What finally worked for me was a fativorous paleo diet. Only after fixing my nutrition did physical exercise became easy and enjoyable.
Given the scarcity of perennial sweet foods in our paleolithic past, and given the (presumedly) evolutionary cues to gorge on such an energy cache, it comes as no surprise that willpower will eventually fail in the face of such a driver – particularly if the individual concerned is well-fed but malnourished.
I have to say that I really look forwards to your post each week. Very much appreciated.
i think your posts are all fine, but then i’ve been reading up on nutrition from this stance for 4-5 years started with Fathead movie blog, then onto robb wolf, MDA, GCBC, then fathead movie, followed some of WAPF, read primal body primal mind, robb wolfs book, primal blueprint, WWGF etc etc
and it all adds layers to your understanding but then trying to pass that information on in a bite sized portion (normally in like 5 minutes of conversation) is practically impossible.
especially when the other person believes the government knows all and are not themselves beholden to corporations etc etc.
but again the person i referred to refuses to try/learn stuff, i meet these people a lot.
I am so going to use this line in discussions with people: “you can’t fix your car by removing the “Check Engine” light.”
It is a perfect analogy to so much of the modern medical field.
I won’t claim it as my own. Don’t sue me.
About a “For Begginers” section, I realise you were thinking about lower science density, but I think the article about meat rotting is really good, in the sense that it shoots down a commom missconception very well, shows there’s a lot of bad information out there and that you’re not just spitting things out and should be generally engaging for anyone actually interested.
It’s a good way to make people start questioning instead of writting you off as some crazy guy making things up.
Also, in my opinion you shouldn’t care too much about people who want it very simple right now, as I kind of doubt they’d buy into it before it gets much more popular.
Chris:
AFAIK at least two of the “blood types” are advised to eat basically paleo. And AFAIK it's also baloney.
Tim:
We're all still stuck in the failed Cartesian mind/body duality mindset. The brain is an organ. It uses energy. And yes, we all know intuitively that stress and difficult decisions make it harder to stay on a diet…but it's good to know that the parsimonious explanation (willpower takes energy) is, in fact, correct.
Asclepius:
I'll be going much more deeply into those topics next week.
eddie:
Everything ties together. One piece of paleo knowledge in isolation can sound like a conspiracy theory…it's tough to explore a single topic and have it make sense.
James:
Please use it! I'm glad it helps.
Fmgd:
Yes, that's a good one for beginners. Someday I should do a succinct debunking of the common vegetarian arguments (“carnivores have claws”, “humans have a long intestine”, etc.) There are some good book-length debunks, but no short, succinct ones that I know of.
JS
J. Stanton said:
Agreed. I just found it interesting because another study brought up the link of DNA and optimal diet here: http://now.tufts.edu/articles/dna-diet
That’s a great idea, it’s a good way to make people stop and listen and it should bring lots of hits.
I think that if there’s anything to a blood type diet it lies in finding clues to what keeps an individual person’s GI tract happy and what makes it unhappy–what is more likely to lead to a leaky/permeable gut in one person versus another. The ideas Peter D’Adamo set forth are too easily dismissed and the one guy I saw try to do it by appealing to some scientific fact has since strongly discredited himself in my eyes so as far as I’m concerned, we’re back to square one.
I have more respect for someone who goes, “Hm, we should test some of these ideas and see if they hold up,” than someone who says, “Oh, that’s B.S., everyone knows that isn’t true.” Show me the evidence or STFU, is the way I see it. Saying “there is no evidence” is not enough–I wouldn’t begin to know where to look for it in the first place!
I’ve actually read D’Adamo, and one thing people claim about him that isn’t true is that he says type As are supposed to be vegetarian. What he actually said was type As *do better* as vegetarians. But whenever I see that misquoted I know to not take the detractor seriously, even if it turns out D’Adamo is totally wrong. Just like the people who talk trash about Dr. Atkins and then claim he said to eat burgers and bacon and cheese and nothing else.
This is an awesome series of yours, by the way. I refer people to your stuff from time to time.
Oh, another thought about blood type diets: At the end of the day, nobody has time to fine-tune what foods are absolutely perfect for their DNA, blood type, metabolic type or whatever. If a dietary approach doesn’t help *generally*, without having to add any weird ingredients or weigh portions, it’s probably not worth following.
In that sense I find a Paleo or Primal approach more valuable than a blood type approach–and a willingness to self-experiment and indulge in an occasional lab test to be even more valuable. I’ve heard it said that people with an engineer’s mindset are better capable of regaining lost health and losing excess fat. I believe it.
Dana:
Thank you! I think there is a lot of confusion right now around this subject, because many people don't realize that “hunger” is the end product of several motivations. And I try very hard to make sure my articles are understandable to people who aren't already part of the paleo world…please keep forwarding them on!
As far as the blood type stuff, I suspect that there are probably some correlations, because there are plenty of genetic variances in amylase, PEMT, apoE, ability to process beta-carotene, etc…but my intuition is that in a time of massive race mixing and genetic flow, those correlations to blood type are going to be quite loose, and a lot of digestive differences are probably due to gut flora. It's a great marketing tool, though: “you're special, you deserve a special diet just for you”.
But like I said, this is all AFAIK, as I haven't read it.
Chris:
Directly looking at known genetic loci seems a lot more valid to me than blood type. But I'm more interested in optimality than in “what can I get away with because of my genome”.
Fmgd:
I'll work on it.
JS
Dana said:
Spot on Dana. You read my mind.
I'm not 100% against 'weighing portions' only because some people have a skewed perception of what “normal” is in America. Weighing for a while gives them a better idea.
Hmm… interesting. I’ve been experimenting with Intermittent Fasting which has mainly worked out as me skipping breakfast. In my food spreadsheet (yes, I’m monitoring, but not necessarily restricting… definitely eating to satiation and eating lots of saturated fats), I began to note that in the mornings if I tried to ignore hunger for an hour or so after I felt it, I would start to have a physiological response similar to the feeling you have right before crying. I wasn’t in an emotional state, so it was interesting to note that the sensations were similar. Finally, I would eat and then feel happy.
I’m experimenting with monitoring right now, but I also will see how I feel when not writing everything down.
Chris:
“Serving sizes” are a joke. Tiny bags of chips contain two “servings”, and people don't realize that meals at your average family restaurant contain over 1000 calories…sometimes over 2000 if you order an appetizer!
Ruby:
Very interesting! I wonder if it's a cortisol spike?
Also, I'm not into pathological use of fitday, but it's definitely worthwhile to record and chart out a few typical days. Often our perception of what we're eating is different from what we're actually eating. It's like any other habit: being mindful of what we do, instead of simply going through each day on automatic reflexes, is very important.
JS
JS:
Exactly. I don't believe so much in serving sizes so much as people knowing how much they're consuming overall.
Plus, have you ever been to Cheesecake Factory?! Last time I was there, a few years ago, their 'chicken breast' entree could have fed three of me! (And that's saying a lot.)
Chris:
I eat out very infrequently. Do I really want a parsimonious little pile of meat floating on a lake of starch and seed oil? No, I don't. There are a limited number of places I can even sate my hunger for actual food, let alone at a reasonable price.
JS
JS:
Definitely. I try not to, but not everyone likes eating the way I (we) do. Even if I offer to cook for them! Oh well. Like you, I don't eat out that much as well.
[…] by knightofalbion Other studies have repeatedly shown frugal eating to be key to longevity. Restrained Eating: Willpower and Why Diets Fail (Why Are We Hungry? Part III) this useful blog post explains why most people can't stand being hungry all the time. The key to […]
Yes, J. Stanton, you should be very proud of this, says the “Cortisol Queen” whose greatest hurdle in 90lbs of weightloss maintained for 9+ years, has been learning to manage the cortisol!
Excellent!
mem:
The mainstream underappreciates the role of cortisol in weight management. Fortunately the paleosphere doesn't, as much: Robb Wolf emphasizes it in his book, for one. It's rare to see a controlled study that so neatly demonstrates the relationship between cortisol and appetite.
Note that people with cortisol issues usually do better by eating protein soon upon waking, e.g. Kruse's leptin reset. (Although Jack is awesome, I find 50g of protein a suspiciously round number that is probably far too much for most people.)
JS
[…] allowed to eat”. We fall back on will power and then it begins to get really tough because will power alone will always let you down. . For me, eating paleo brings with it a profound sense of […]
[…] Paleo Corner – Restrained Eating: Willpower and Why Diets Fail (Why Are We Hungry? Part III) […]
I think Vitamin C deserves a mention on this page. You can’t burn fat without it, and the diet you propose is seriously deficient in C.
Here is just some of the papers to spark your interest:
http://goo.gl/OueXH
Also, check out how C supplementation goes nicely with low carb diet:
Ascorbic Acid and the Immune System
http://goo.gl/B8o21
majkinetor:
How is the diet I propose deficient in vitamin C?
Also, there are major problems with vitamin C supplementation, especially if you're active:
“Antioxidants prevent health-promoting effects of physical exercise in humans”
http://www.pnas.org/content/early/2009/05/11/0903485106.abstract
“Oral administration of vitamin C decreases muscle mitochondrial biogenesis and hampers training-induced adaptations in endurance performance”
http://www.ajcn.org/content/87/1/142.long
JS
Because meats don’t have C. Eyes, brainz, adrenals and such are the organs containing C, alas, nobody eat those. Then, since most of the fruit is out of the question and plants don’t need vitamin C a lot, you can easily become seriously deficient. Other sources of C are probably destroyed via cooking or storage.
High fat diet also probably makes endotoxin load greater and endotoxins can be completely detoxified with vitamin C, etc.
Adrenals require Vitamin C a lot, and any stress during this diet, including the stress of the diet itself which is typical for the starters will remove all remaining vitamin C stores from the tissues.
I am aware of the few studies linking vitamin C supplementation and reduced response to exercise, but, there are hundreds other showing different results. Even if true, its more important to prevent injuries then to build muscles optimally. Also, excercise also produces endotoxin burden. You need to look at the whole picture.
I find it silly to question vitamin C in exercise to be honest, since all animals except humans and friends don’t make it and I don’t think natural predators are having problems in that manner :), all optidosing much higher level of C via liver or kidnies.
While I appreciate the source of your info (gettingstronger, great site for hormesis research) its highly biased in some moments. Most of the studies referenced in that page are rebutted multiple times so far and picking up few that are negative is nothing else but citation bias.
majkinetor:
As far as “meats don't have vitamin C”, that's true…but 1) an
all-meat diet doesn't appear to result in deficiency (see: Stefansson), only a “mostly
meat” diet, and most importantly 2) I don't advocate an all-meat diet!
As I've noted repeatedly, my vegetable intake has gone up since upping
my meat/egg intake and removing grains. I don't push people to consume
vegetables, because you'll naturally find yourself desiring them once
the empty starches are gone.
Can you point me to rebuttals of the studies which show a blunting of the exercise response? I'd like to see them, because they seem very solid to me. The mechanism seems simple: exogenous antioxidants trick the body into not performing its own free radicalscavenging and damage repair…but I'm open to correction here.
Furthermore, I strongly disagree with your characterization of that blunting as unimportant. It's not just building muscles — it's improving our endurance via increased mitochondrial efficiency and capacity. I don't just enjoy going out and doing long hikes or long rides because of the ride itself: I enjoy them because they make me more capable of going to even more interesting places in the future! I'm not interested in just being alive a bit longer, I'm interested in being the best I can be and doing the most I can do. And I know from experience that I'm dramatically less stressed when I'm accomplishing things than when I'm stuck in a rut.
Also, I think we have to be careful assuming that since most animals make a lot of endogenous vitamin C, that humans and great apes need just as much. In order to compensate, we've evolved very efficient recycling machinery for the vitamin C we do ingest…so there's no direct dose equivalence between what they make and what we require.
Purely as anecdotal evidence, I had a doctor a long time ago that was into megadosing Vitamin C for all sorts of issues, and it never gave me anything but the farts when I hit bowel tolerance. So while I agree that deficiency, including subclinical scurvy, may be an issue (yes, I follow and respect the Jaminets) I don't see a reason to destroy our body's ability to adapt to its environment for the putative health benefits of megadosing. But again, if you've got references to controlled trials that show solid benefits to high doses of Vitamin C, I'm all ears.
JS
[…] Restrained Eating: Willpower and Why Diets Fail (Why Are We Hungry? Part III) September 9, 2011By: J. Stanton Read the Full Post at: GNOLLS.ORG […]
The Impact of Weight Stigma on Caloric Consumption These findings suggest that among overweight women, exposure to weight stigmatizing material may lead to increased caloric consumption.
Ted:
That makes sense. When pounded with negative stimulus, people will naturally seek out a compensating positive stimulus — in this case, the reward of snack food. People strongly seek out a certain amount of reward in their life…
…which is why I don't believe that “just eat bland food” is a good long-term solution. Reward restriction has similar problems as calorie restriction: just as calorie restriction doesn't address the metabolic problems that caused us to become obese, reward restriction doesn't address the underlying problems that drive us to seek reward through food.
Thank you for the reference!
JS
J. Stanton, in the paragraph “When willpower fails”, you refer to “endless hours of practice” in an attempt to explain why our PFC isn’t in control of our actions. I will attempt to point out why this is more confusing than anything else.
Practice is the act of repeating systematically for the purpose of developing, improving and maintaining skill. Have you ever seen pros practice their techniques in slow motion? They are not practicing old motions here, they are developing new ones. Everything with any degree of complexity like sports, music and martial arts require lots of practice, but most importantly require one to learn the motions slowly at first just to learn them, and to learn them properly. This is nothing to do with the activity itself but with how we learn new motions. We learn motions independently of speed. Rather, we can’t learn new motions at full speed especially complex motions like playing the piano (multiple fingers and the feet work simultaneously) or the drums, fighting (legs, feet, hands, eyes, etc, all working together and simultaneously again) or basically any motion that requires more than the simple push of a button. When we try to learn those new complex motions, the old ones take over. This is probably why it gives the impression that we (our PFC) are not in control of our actions.
It occurred to me that our PFC might act in a similar fashion as flash memory. It’s slow to put stuff in, but once it’s in, it’s quick to read it back. Rather, _slow_ means “to put stuff in”, and _fast_ means “to read it back out”. So when we try to learn motions at full speed, since it’s fast, we default to “read back what was written previously”, when what we really want to do is “overwrite what’s already in there with something different”.
Anyway, this is why I think that your reference to endless hours of practice is more confusing than anything else with regards to our PFC, willpower and hunger.
Martin:
As a musician and sportsman, I'm intimately familiar with the issues of skills practice.
I believe your point is that the PFC can maintain control if we move slowly enough, which is often true (although some motions can't be performed in slow motion due to the constant nature of gravity and the viscosity of air). However, often even slow-motion isn't enough, and we need to break down motions into smaller and simpler parts that can be commanded by the PFC. Even something as simple as hitting a drum with a drumstick involves a surprising sequence of finger motions that isn't obvious to the observer (it involves the little and ring fingers) and must usually be demonstrated and learned by parts.
However, the PFC isn't in control at real-time speeds. What we call “muscle memory” is how we learn these new motions: whether hitting a drum, throwing a punch, or kicking a ball. I don't think it's an issue of slow in/fast out: I believe that the structure of the brain (the forebrain is a thin layer on top of everything else, including the sensory and motor cortex), as well as the experience of millions, argues that motions are learned by these deeper brain structures and triggered/commanded by the PFC.
Further, I believe the “slow input” is a matter of retraining these deeper structures to respond appropriately: instead of cringing when someone throws a punch, we can train ourselves to slip it or block it. But this takes time and repetition — otherwise known as “practice” — which proves to me that real-life skills are not under direct control of the PFC.
JS
That’s partly my point, yes. I hadn’t thought of a more appropriate example to use instead of practice, but now I do: Sex. I think it’s a much more appropriate parallel for the point you were trying to make about willpower. In this case, “Why Willpower Fails When You’re Hungry With Food In The Fridge” could as easily be replaced with “Why Condoms Are Useless When You’re Naked And Ready And In Pleasant Company”. It would require every ounce of willpower to resist indeed.
But my point was that the apparent of lack of control when playing the piano for the first time is a completely different nature than the lack of control found when hunger is involved, and so a parallel between the two can’t be drawn so easily.
Martin:
You're correct that it's not good to push an analogy too far.
However, my point wasn't to liken hunger to practicing music: it was only to demonstrate that we're not perfectly rational beings whose drives are completely under our own conscious control. I hope that much was clear.
JS
And yet practicing can also be applied to eating successfully. I successfully managed my weight for decades with chronic restrained eating. It became unconscious second nature and I did not feel deprived. I simply did not take second helpings and passed on things I knew were not good for me. It’s not a whole lot different than adopting a paleo diet, either. This, too, requires willpower and a certain degree of fore-planning. The food itself may be more satiating but it takes a degree of willpower not to eat poorly in many situations and takes a great deal of PFC action to make good choices up-front, especially in our culture. Try attending a potluck sometime and see if your willpower muscle gets a little usage.
Diane:
That's an interesting perspective: restrained eating as a learnable skill.
JS
“In other words, we shouldn’t have to be hungry all the time in order to stay healthy and fit.”
I’m still trying to reconcile my desire for that to be true while I’m trying to lose weight with my personal experience that I have to feel some hunger all the time to actually lose weight.
CaptRover:
I can't possibly debug that statement without knowing what you're eating and when.
JS
The key thing CaptRover is to stop all snacking. Snacking between meals screws up the hunger hormones.