Favorite Articles of the Moment
Disclaimer
• Your life and health are your own responsibility.
• Your decisions to act (or not act) based on information or advice anyone provides you—including me—are your own responsibility.
Recent Articles
-
We Win! TIME Magazine Officially Recants (“Eat Butter…Don’t Blame Fat”), And Quotes Me
-
What Is Hunger, and Why Are We Hungry?
J. Stanton’s AHS 2012 Presentation, Including Slides
-
What Is Metabolic Flexibility, and Why Is It Important? J. Stanton’s AHS 2013 Presentation, Including Slides
-
Intermittent Fasting Matters (Sometimes): There Is No Such Thing As A “Calorie” To Your Body, Part VIII
-
Will You Go On A Diet, or Will You Change Your Life?
-
Carbohydrates Matter, At Least At The Low End (There Is No Such Thing As A “Calorie” To Your Body, Part VII)
-
Interview: J. Stanton on the LLVLC show with Jimmy Moore
-
Calorie Cage Match! Sugar (Sucrose) Vs. Protein And Honey (There Is No Such Thing As A “Calorie”, Part VI)
-
Book Review: “The Paleo Manifesto,” by John Durant
-
My AHS 2013 Bibliography Is Online (and, Why You Should Buy An Exercise Physiology Textbook)
-
Can You Really Count Calories? (Part V of “There Is No Such Thing As A Calorie”)
-
Protein Matters: Yet More Peer-Reviewed Evidence That There Is No Such Thing As A “Calorie” To Your Body (Part IV)
-
More Peer-Reviewed Evidence That There Is No Such Thing As A “Calorie” To Your Body
(Part III)
-
The Calorie Paradox: Did Four Rice Chex Make America Fat? (Part II of “There Is No Such Thing As A Calorie”)
-
Interview: J. Stanton on the “Everyday Paleo Life and Fitness” Podcast with Jason Seib
|
(This is a multi-part series. Go back to Part I, Part II, or Part III.)
Empirical Evidence: Greater Weight Loss And Fat Loss On Isocaloric High Protein Diets
Dozens of studies have demonstrated that high-protein diets result in greater loss of bodyweight and fat mass than isocaloric lower-protein diets. (Isocaloric = containing the same number of “calories”.)
Instead of bombarding you with citations, I’ll point you to references 11 through 44 (and 2) of this excellent paper:
Nutr Metab (Lond). 2012 Sep 12;9(1):81. doi: 10.1186/1743-7075-9-81.
Dietary protein in weight management: a review proposing protein spread and change theories.
Bosse JD, Dixon BM.
(Fulltext available here.)
While some will critique that the satiating effect of higher dietary protein sometimes results in voluntary hypophagia [11], leading to an energy intake discrepancy between groups, there is evidence that increased dietary protein leads to improved body composition and anthropometrics under iso-, hypo-, and hyper-caloric conditions [2, 11-44]. Thus, the traditional dogma of “energy in versus energy out” explaining weight and body compositional change is not entirely accurate.
Now, it’s quite possible to pick a fight by cherry-Googling a few studies that show no advantage to high-protein diets. CITATION WAR!!11!!!1 Who’s right?
Rule Of Thumb: When there is a wide spread of outcomes, it’s likely that other factors, besides the one being studied, are influencing the results.
For instance, there are studies showing that calcium supplementation increases weight loss, and studies showing it does not. Instead of arguing that the studies opposing one’s hypothesis must all be flawed or fabricated, it’s more productive to look for other factors…
…and indeed, we find that calcium supplementation only increases weight loss if one is calcium-deficient to begin with.
Br J Nutr. 2009 Mar;101(5):659-63.
Calcium plus vitamin D supplementation and fat mass loss in female very low-calcium consumers: potential link with a calcium-specific appetite control.
Major GC, Alarie FP, Doré J, Tremblay A.
The application to such controversies as “Is there a metabolic advantage to low-carb diets?” should be obvious.
First, we know that a host of factors besides protein intake influence weight and fat mass (some of which I discussed in Part II and Part III). Furthermore, the dozens of studies in question prescribed a wide range of diets—anything from nutrient shakes to nuts to protein supplements to prepared meals to “we give you dietary advice; you keep dietary records and we’ll analyze them for compliance”—so we would rightly expect some of these changes to influence study outcomes. Unfortunately, it’s difficult to discern patterns across such a wide range of variables.
However, Bosse and Dixon have found two factors that can easily be compared between studies: protein spread and protein change.
Protein spread is the difference in protein content between low- and high-protein diets; protein change is the difference in protein content between a test subject’s habitual diet and the high-protein diet.
“In studies where a higher protein intervention was deemed successful there was, on average, a 58.4% g/kg/day between group protein intake spread versus a 38.8% g/kg/day spread in studies where a higher protein diet was no more effective than control. The average change in habitual protein intake in studies showing higher protein to be more effective than control was +28.6% compared to +4.9% when additional protein was no more effective than control. Providing a sufficient deviation from habitual intake [“protein change” -JS] appears to be an important factor in determining the success of additional protein in weight management interventions.” (Ibid.)
Even more striking, when the authors excluded studies in which the protein content of the low-protein diet was insufficient to meet the RDA, the mean difference in spread increased from 19.6% to 21.7%, and the mean difference in change increased from 23.7% to 37%!
 Figure 2, Protein spread  Figure 3, Protein change
For those skeptical about the ranges in the above graphs: “…There appeared to be plausible explanations for nearly all outliers.” (Ibid.) Read the Discussion section if you’re interested in the details.
For instance: “A flaw in previous trials was that at times higher protein groups consumed more protein than control, yet less than their habitual intake, and saw no difference in anthropometrics [33, 52, 57, 61]. Thus, the “intervention” diet was really not an intervention to their metabolism. […] In some cases, increasing the % of kcals from protein during energy restriction can actually result in less protein being consumed during intervention than habitual intake as a simple function of energy deficit.” (Ibid.)
For example, if you design a 1000-“calorie” diet for someone whose habitual intake is 1900 “calories” with 15% protein, you’ll have to include 28.5% protein just to give them the same amount of protein they were getting before.
“What is the protein spread on this study?” and “What is the protein change in this study?” are common-sense questions to ask. If protein spread is too small, the diets will be too similar to cause significantly different outcomes. If protein change is too small, the “high-protein” diet won’t be different enough from a subject’s habitual diet to cause a significantly different outcome. So while other factors are very likely to influence the outcome, it’s clear that protein change (and, to a lesser extent, protein spread) account for most of the difference between outcomes in high-protein dietary interventions.
Conclusion: A calorie is not a calorie when you consume it as protein instead of fat or carbohydrate.
Our Story So Far
- A calorie is not a calorie when you eat it at a different time of day.
- A calorie is not a calorie when you eat it in a differently processed form.
- A calorie is not a calorie when you eat it as a wholly different food.
- A calorie is not a calorie when you eat it as protein, instead of carbohydrate or fat.
- Controlled weight-loss studies do not produce results consistent with “calorie math”.
And, therefore:
- Calorie math doesn’t work for weight gain or weight loss.
What happens if we decide to “count calories” anyway? Continue to Part V, “Can You Really Count Calories?”.
(This is a multi-part series. Go back to Part I, Part II, or Part III.)
Live in freedom, live in beauty.
JS
“A wonderful, inspired, original, inspiring story…A cry of joy and terrifying beauty, an extraordinary commentary on the human condition, something that can change the way you see the world and your place in it…
…This book reflects some of the deepest teachings from Tibetan Buddhism; the fearless radical insight of Dorje Drollo, speaker of the Three Terrible Oaths…
…Evokes a direct and total engagement with life, and explains why hyenas laugh. READ IT!!!”
Yes, this is a review of The Gnoll Credo.
If you haven’t yet read it, ask yourself: what value might I place on such an experience? I suspect it exceeds $10.95 US…so click here and buy one.
Thank you.

Even after the previous installment of this series, there are still people who believe that calorie intake—and calorie output via exercise—are the only factors that affect weight loss. Apparently my work is not done!
(This is a multi-part series. Go back to Part I, Part II.)
Empirical Evidence: A Calorie Is Not A Calorie When You Add Lots Of Coconut Oil Or Butter To Your Regular Diet
Take three groups of Wistar rats. One group gets free access to standard low-fat rat chow; the others get free access to both standard chow and a “high-fat chow”, 2/3rds of which is butter or coconut oil. (Hat tip to George Henderson for this one.)
Nutr Metab (Lond). 2007; 4: 4.
Long term highly saturated fat diet does not induce NASH in Wistar rats
Caroline Romestaing, Marie-Astrid Piquet, Elodie Bedu, Vincent Rouleau, Marianne Dautresme, Isabelle Hourmand-Ollivier, Céline Filippi, Claude Duchamp, and Brigitte Sibille
(Note: link is to fulltext.)
A fourth group of rats in this study ate a methionine- and choline-deficient diet, which was the primary subject of the study (a successful attempt to give rats fatty liver). Short version: deficiencies caused fatty liver, but massive fat ingestion (and “calorie surplus”) did not.
Unsurprisingly, the rats with free access to the rat version of buttered popcorn ate it. By the end of the diet, both the coconut and butter groups were consuming slightly more high-fat chow than regular chow, the butter group was consuming 30% more “calories” than the chow-only group, and the coconut oil group was consuming 140% more “calories” than the chow-only group!
If a calorie is a calorie, we would expect the rats to gain fat roughly in proportion to their calorie intake. Here’s what actually happened, from Figure 1:
 Figure 1 from Romestaing et.al.
The open triangles and dashed line represent the chow-only rats, the gray circles and solid line represent the butter+chow rats, and the black circles and solid line represent the coconut oil+chow rats. Results: “Surprisingly, in spite of a larger energy intake, body mass was not affected in rats fed the high fat diets.” The chow+coconut oil rats ate 2.4 times as many “calories” as the chow-only rats—
—and gained exactly the same amount of weight.
Even the butter+chow rats ate 30% more “calories”, but gained only a non-significant amount of extra weight.
Errata?
Note that the graph above is partially incorrect: Table 3 gives calorie counts for each group, which agree with the figures quoted in the Results section but disagree with the graph. Apparently the calorie curve for the chow-only rats is shifted upwards, and the calorie curve for the butter+chow rats is just plain wrong! (Or Table 3 is wrong…I’ll pass on any additional information I find.)
Why It’s Important To Report Absolute Change, Not Just Relative Change
The study makes much of the extra WAT (white adipose tissue) gained by the coconut oil+chow rats—62% more—but as the rats started with very little fat, the total gain was approximately 8.4g versus 5.6g for the chow-only rats, for a difference of appx. 2.8g of fat on a 450-gram rat.
In human terms, that’s a 0.6% difference in bodyfat percentage…just under a pound for a 160-pound human.
This, gentle reader, is why it’s important to look at absolute percentages, not just relative percentages…a 62% increase in almost zero is still almost zero. (And this is why so many drug trials report relative risk…a 40% decrease in mortality sounds great until you discover that your absolute risk dropped from 1 in 200 to 1 in 333. Meanwhile, the chance of harmful side effects has stayed the same—and it’s usually far greater than the chance of being saved.)
Conclusion: A calorie is not a calorie when you add lots of coconut oil or butter to your regular diet.
Empirical Evidence: A “Calorie” Of Almonds Does Not Equal A “Calorie” Of Complex Carbohydrates
Take 65 obese and insulin-resistant people. Divide them into two groups, and place each group on a different 1000-calorie starvation diet for 24 weeks. (Another hat tip to Kindke for bringing this one to my attention.)
Int J Obes Relat Metab Disord. 2003 Nov;27(11):1365-72.
Almonds vs complex carbohydrates in a weight reduction program.
Wien MA, Sabaté JM, Iklé DN, Cole SE, Kandeel FR.
(Fulltext available here.)
The study subjects were in bad shape. Mean BMI: 38, weight: 250# (113kg), fasting blood glucose: 152 mg/dl, fasting insulin: 46 ulU/ml (320 pmol/l). Note that a reasonable fasting glucose measurement would be <100 mg/dl, and reasonable fasting insulin would be <9 ulU/ml...so these subjects exhibit classic signs of the metabolic syndrome in addition to being obese.
Now, here comes the interesting part: Just over half the 1000 calories were fed as either "self-selected complex carbohydrates" ("peas, corn, potato, pasta, rice, etc.") or as unsalted, unblanched almonds. I'll skip to the punchline:
[caption width="400" align="aligncenter"] Figure 2 of Wien et.al.[/caption] Figure 2 of Wien et.al.[/caption]
That’s 43 pounds lost (19.5kg) for the almond group versus 26.6 pounds lost (12kg) for the complex carbohydrate group.
The authors quote, with typical scientific understatement: “The difference in weight loss was unexpected, given the study design featuring a matched prescribed total calorie intake and equivalent levels of self-reported physical activity between the groups.”
Furthermore, we can see that the “complex carbohydrate” group had plateaued by week 16 (92% of total weight loss after 67% of the time), whereas the almond group was continuing to lose weight at the end of the study (only 77% of weight loss after 67% of the time).
“Calorie math” says that to lose 16.4 more pounds, the almond group would have to have eaten 340 fewer “calories” per day…that’s 2/3rds of the “calories” in the almonds!
Even if we only count the 11.1 pound difference in fat mass lost (see Table 3), “calorie math” requires the almond group to have eaten 230 fewer “calories” per day.
Yet the subjects were voluntary inpatients at a medical clinic, where access to food was controlled. Additionally, “Subjects did not differ in their self-reported evaluation of the acceptability of their assigned dietary intervention in terms of satiety, palatability and texture at weeks 0, 8, 16 and 24,” and “Both groups had equivalent levels of noncompliance…during the 24-week intervention.” So cheating by either group seems unlikely, unless you posit that almonds give you the magical ability to jog for half an hour every day without anyone else noticing—and lie about it.
There were dramatic improvements in health markers for the almond group, which I’ll leave as an exercise for my readers. (Hint: see Table 3.)
Conclusion: A “calorie” of almonds does not equal a “calorie” of complex carbohydrates.
Our Story So Far
Using peer-reviewed science and publicly available population-level statistics, we’ve proven that:
- A calorie is not a calorie when you eat it at a different time of day.
- A calorie is not a calorie when you eat it in a differently processed form.
- A calorie is not a calorie when you eat it as a wholly different food.
- Controlled weight-loss studies do not produce results consistent with “calorie math”.
And, therefore:
- “Calorie math” doesn’t work for weight gain or weight loss.
The juggernaut continues to roll! Continue to Part IV, Protein Matters…and feel free to stir up some controversy by sharing this article with the widgets below.
Live in freedom, live in beauty.
JS
(This is a multi-part series. Go back to Part I, Part II.)
Thanks to everyone who places their Amazon.com orders through my affiliate link: you’re supporting gnolls.org at no cost to yourself. So next time you’re placing an order for books, music, video games, TVs, cooking implements, or anything else, please consider starting here, or at the link in the right sidebar. (Which takes you to the page for The Gnoll Credo—but you can order anything you want, and it’ll still help support gnolls.org.)
To those worried about privacy: no, I have no way to find out who ordered what.

It’s possible to “prove” just about anything via a blizzard of citations and a few carefully-placed appeals to authority. It’s also easy to become seduced by a plausible and elegant biochemical pathway. Presto: science!
However, when formulating a hypothesis, it’s most important to constrain it by observed reality.
(This is Part II of a series. Click here for Part I.)
Empirical Evidence: “Calorie Math” Doesn’t Work
“ERS data suggest that average daily calorie intake increased by 24.5 percent, or about 530 calories, between 1970 and 2000.” (Source: “Profiling Food Consumption In America”, USDA Economic Research Service.) In absolute terms, the average American was consuming roughly 2150 “calories” per day in 1970, 2260 “calories” per day in 1980—and nearly 2700 “calories” per day in 2000.
 Source: USDA ERS Note that the shape of this curve roughly parallels the prevalence of obesity in America, which increased slowly before 1980 and took a steep upturn afterwards:
 Note that the upturn in obesity coincides with the US Government’s advice to eat less fat and cholesterol, and more whole grains. Edible fats contain roughly 3500 calories per pound. Therefore, assuming that people were close to their mythical “daily maintenance calories” in 1970, “calorie math” tells us that the average American gained approximately 800 pounds between 1970 and 2000…and has been gaining one pound per week ever since!
 If “calorie math” worked, we would all look like this. Meanwhile, back in reality, the average adult American gained approximately 19 pounds between 1971 and 2000. (Source: Mean Body Weight, Height, and Body Mass Index, United States 1960–2002, Centers for Disease Control.)
The same “calorie math” says a 19-pound gain in 30 years should require a surplus of just six calories per day. That’s nearly two orders of magnitude smaller than the observed 530 calories per day.
Yes, six calories is enough to stop the obesity crisis! All Americans have to do in order to stop gaining weight is to pull four Rice Chex out of the bowl each morning.
 I blame the ones hiding under the spoon. Clearly, “calorie math” doesn’t work.
These are back-of-the-envelope calculations, and are not meant to be exact. And I know some might be tempted to quibble about potential errors in the ERS data: keep in mind that we’re not speaking of a 12% difference, or even a 100% difference. We’re speaking of a nearly 10,000% difference between predicted and observed weight gain.
Yes, I weighed the Rice Chex myself.
Empirical Evidence: “Calorie Math” Doesn’t Work, Part II
We’ve established that the 3500-calorie rule is off by roughly two orders of magnitude for weight gain. It’s also wildly inaccurate for weight loss.
Int J Obes (Lond). 2013 Apr 8. doi: 10.1038/ijo.2013.51. [Epub ahead of print]
Can a weight loss of one pound a week be achieved with a 3500-kcal deficit? Commentary on a commonly accepted rule.
Thomas DM, Martin CK, Lettieri S, Bredlau C, Kaiser K, Church T, Bouchard C, Heymsfield SB.
Despite theoretical evidence that the model commonly referred to as the 3500-kcal rule grossly overestimates actual weight loss, widespread application of the 3500-kcal formula continues to appear in textbooks, on respected government- and health-related websites, and scientific research publications. Here we demonstrate the risk of applying the 3500-kcal rule even as a convenient estimate by comparing predicted against actual weight loss in seven weight loss experiments conducted in confinement under total supervision or objectively measured energy intake.
Their Java applet simulates the average of all the weight vs. time curves extracted from the studies they selected: you can download it here. While it doesn’t account for the differences caused by macronutrient composition (e.g. Ludwig 2012), meal timing (see below), meal composition (see below), or the host of other significant factors, you can amuse yourself by turning on “Show 3500 Calorie Rule” from the Options menu.
Clearly, “calorie math” doesn’t work.
Empirical Evidence: A “Calorie” At Dinner Does Not Equal A “Calorie” At Breakfast
Here’s a fascinating controlled study:
Obesity (Silver Spring). 2011 Oct;19(10):2006-14
Greater weight loss and hormonal changes after 6 months diet with carbohydrates eaten mostly at dinner.
Sofer S, Eliraz A, Kaplan S, Voet H, Fink G, Kima T, Madar Z.
Seventy-eight police officers (BMI >30) were randomly assigned to experimental (carbohydrates eaten mostly at dinner) or control weight loss diets for 6 months.
[…]
Greater weight loss, abdominal circumference, and body fat mass reductions were observed in the experimental diet in comparison to controls. Hunger scores were lower and greater improvements in fasting glucose, average daily insulin concentrations, and homeostasis model assessment for insulin resistance (HOMA(IR)), T-cholesterol, low-density lipoprotein (LDL) cholesterol, high-density lipoprotein (HDL) cholesterol, C-reactive protein (CRP), tumor necrosis factor-α (TNF-α), and interleukin-6 (IL-6) levels were observed in comparison to controls.
[…]
A simple dietary manipulation of carbohydrate distribution appears to have additional benefits when compared to a conventional weight loss diet in individuals suffering from obesity.
How about that?
The officers were eating the same number of “calories”…they were even eating the same balance of protein, fat, and carbohydrate. Yet, the “carbs for dinner” group lost an additional 2.5kg (5.5 pounds) after six months.
Furthermore, this was a deeply restricted diet (1300-1500 “calories”), so we’d expect all the participants to be extremely hungry. (The Minnesota Starvation Experiment fed its volunteers more: 1600 “calories” per day.) Yet the “carbs for dinner” group rated themselves as less hungry and more sated…so real-world results, in which food intake is only restrained by one’s willpower, would be even greater.
Finally, the “carbs for dinner” crowd were healthier in all measured respects: lower abdominal circumference and fat mass, lower fasting glucose and HOMA(IR), lower LDL, higher HDL, and lower whole-body inflammation (CRP, TNF-α, IL-6). All this from a standard “healthy” high-carb diet (20% protein, 30-35% fat, 45-50% carbohydrate), tweaked so that the carbohydrates were eaten mostly at dinner!
Conclusion: a “calorie” of carbohydrate eaten for breakfast is not equal to a “calorie” of carbohydrate eaten for dinner.
According to “calorie math”, the additional weight loss would equal 107 fewer “calories” per day. Apparently you can change the number of “calories” in food just by eating it at a different time of day…
…or perhaps the concept of “calories” is flawed. (I’ll leave the additional problems this experiment poses for reward-based hypotheses of obesity as an exercise for the reader.)
Also note the dramatic alterations to the hormonal milieu: the same authors explore this in more detail in a followup study.
Nutr Metab Cardiovasc Dis. 2012 Aug 14. [Epub ahead of print]
Changes in daily leptin, ghrelin and adiponectin profiles following a diet with carbohydrates eaten at dinner in obese subjects.
Sofer S, Eliraz A, Kaplan S, Voet H, Fink G, Kima T, Madar Z.
Empirical Evidence: A “Calorie” Of Powdered Food Does Not Equal A “Calorie” Of Regular Food
Hat tip to Kindke for this excellent and well-controlled study:
Br J Nutr. 2013 Apr;109(8):1518-27. doi: 10.1017/S0007114512003340. Epub 2012 Aug 6.
Diet-induced obesity in ad libitum-fed mice: food texture overrides the effect of macronutrient composition.
Desmarchelier C, Ludwig T, Scheundel R, Rink N, Bader BL, Klingenspor M, Daniel H.
“The most striking finding was that all mice fed the different powder diets developed obesity with similar weight gain, whereas among the mice fed the pellet diets, only those given the HF and W diets became obese.”
(Note that all mice were fed ad libitum, which means they could eat as much as they wanted.)
Two instructive graphs:
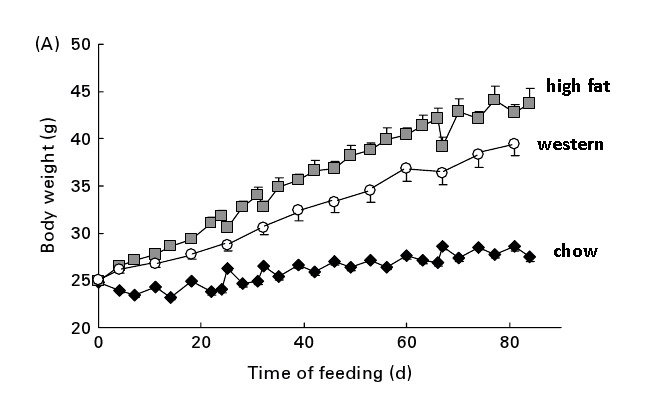 Weight change on standard pelleted diets. See? High-fat diets cause obesity! (In C57BL/6N mice genetically-engineered to quickly become obese.)
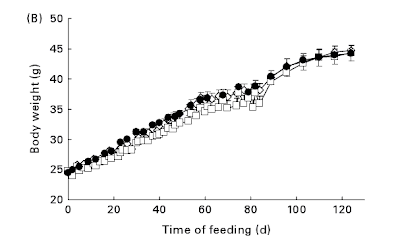 Weight change on powdered diets. Except when you grind them all into powder—at which point all diets become equally “obesogenic”.
Another fascinating fact: the mice who became obese on the powdered chow were eating the same amount of food that kept them lean when it remained in pellet form! Yes, they were eating the same number of “calories”…
…which made them fat in powder form, but not in pellet form.
We’re not just talking about a little bit of extra fat, either: the mice got 80% heavier on the powdered food, versus 18% on the pelleted version of the same food.
Furthermore, the mice who ate the “high-fat” diet consumed 19% fewer “calories” worth of powdered food—but became just as fat as before. And the mice eating the “Western” diet also consumed 19% fewer “calories”—but became even fatter than before!
Conclusion: a “calorie” of powdered food does not equal a “calorie” of regular food—particularly when the powder is primarily carbohydrate.
Some More Observations On Desmarchelier et.al.
As Kindke notes, flour is powdered carbohydrate. So is sugar. So is almost anything that ends up packaged in a brightly-colored box…processed foods are almost entirely comprised of grains ground into powder, pressed into shape, usually doused with sugar, and baked or fried. Bread, cereal, pasta, donuts, cookies, corn chips, crackers, “instant” anything…yet another reason that Step 1 of “Eat Like A Predator” contains “Do not eat anything made with ‘flour’.”
This study also poses several problems for reward-based hypotheses of obesity. The “high-fat” diet became less “rewarding” when ground into powder, but resulted in the same weight gain. The “Western” diets came in three different flavors, but produced identical results…and all became less “rewarding” when ground into powder, yet resulted in more weight gain. And chow was apparently just as “rewarding” in powder form as in pellet form, yet caused much greater weight gain. (For a demystification of the current state of hunger science, watch my AHS 2012 presentation.)
Finally, here’s a bonus observation. Quote from the paper: “Irrespective of the food texture, the W diet induced a more severe hepatosteatosis and higher activities of serum transaminases compared with the two other diets. In conclusion, diets differing in macronutrient composition elicit specific pathophysiological changes, independently of changes in body weight. A diet high in both fat and sugars seems to be more deleterious for the liver than a HF diet.”
There’s much more—including an indictment of the entire field of obesity research, which has based much on the idea that “high-fat” diets cause obesity. Head over to Kindke’s article to read it.
Conclusions: Our Story So Far
- A calorie is not a calorie when you eat it at a different time of day.
- A calorie is not a calorie when you eat it in a differently processed form.
- Calorie math doesn’t work for weight gain or weight loss.
And we haven’t yet discussed the effects of nutrient partitioning, the mysteries of acronyms like REE, TEE, and TEF, or the myriad other ways in which a calorie is not a calorie. Click here to continue to Part III!
Live in freedom, live in beauty.
JS
(This is Part II of a series. Click here for Part I.)
You. Yes, you. The one who doesn’t yet own a copy of The Gnoll Credo.
You saw Fight Club, right? Everyone did. Well, in addition to being “Raw, powerful and brilliant,” “Funny, provocative, entertaining, fun, insightful,” and “Utterly amazing, mind opening, and fantastically beautiful,” The Gnoll Credo also inspires reviews such as “You must read this forthwith—it’s more life changing than Fight Club“…an assessment with which I agree.
So: BUY IT.
Thank you.
|
“Funny, provocative, entertaining, fun, insightful.”
“Compare it to the great works of anthropologists Jane Goodall and Jared Diamond to see its true importance.”
“Like an epiphany from a deep meditative experience.”
“An easy and fun read...difficult to put down...This book will make you think, question, think more, and question again.”
“One of the most joyous books ever...So full of energy, vigor, and fun writing that I was completely lost in the entertainment of it all.”
“The short review is this - Just read it.”
Still not convinced?
Read the first 20 pages,
or more glowing reviews.
Support gnolls.org by making your Amazon.com purchases through this affiliate link:

It costs you nothing, and I get a small spiff. Thanks! -JS
.
 Subscribe to Posts Subscribe to Posts
|
Gnolls In Your Inbox!
Sign up for the sporadic yet informative gnolls.org newsletter. Since I don't update every day, this is a great way to keep abreast of important content. (Your email will not be sold or shared.)
IMPORTANT! If you do not receive a confirmation email, check your spam folder.
|












